A total of 1,422 people in B.C. died of an illicit drug overdose in 2017, marking the most sobering year of drug-related deaths in the province’s history.
That’s roughly seven people dying every two days, according to new data released by the B.C. Coroners Service, summarizing the second year of B.C.’s first-ever declared health emergency.
“It was the most tragic year ever,” B.C.’s chief coroner Lisa Lapointe said during a news conference Wednesday, alongside provincial health officer Dr. Perry Kendall, and Dr. Patricia Daly, executive director of the B.C. Overdose Emergency Response Centre.
READ MORE: Fentanyl-linked overdose deaths soar in B.C.
READ MORE: B.C. launches new drug-checking program, expands fentanyl testing
READ MORE: Five people die from overdoses in just over nine hours in Abbotsford
The powerful opioid fentanyl was detected in 81 per cent of last year’s deaths, compared to about 67 per cent in 2016.
Lapointe said all fentanyl deaths were linked to illegal sources, and without those deaths, only roughly 300 people would have suffered a fatal overdose.
All corners of the province were affected, with 895 people, the lion’s share, dying in the Lower Mainland.
In Vancouver – the city with the highest rate of overdoses – there were 338 deaths, followed by Surrey with 174, and Victoria with 91 deaths.
Central cities in B.C. were hit the hardest, including Kelowna, Kamloops and Prince George.
The B.C. Coroners Service does not release data for communities where fewer than seven people have died from an overdose because of privacy concerns.
How are officials combating overdoses?
The last four months of 2017 saw some relief in the number of deaths, giving health officials hope that new programs are working for some.
The average number of deaths per month between September and December was 96, compared with 129 per month in the first eight months.
In December, 99 people died, compared to the record-breaking 164 the previous December.
B.C. has opened 10 overdose prevention sites – including two mobile sites in Kelowna and Kamloops, as well as three safe consumption sites in Surrey and Vancouver, with a fourth awaiting Health Canada approval in Victoria.
Not a single people has died of an overdose at a safe consumption or overdose prevention site.
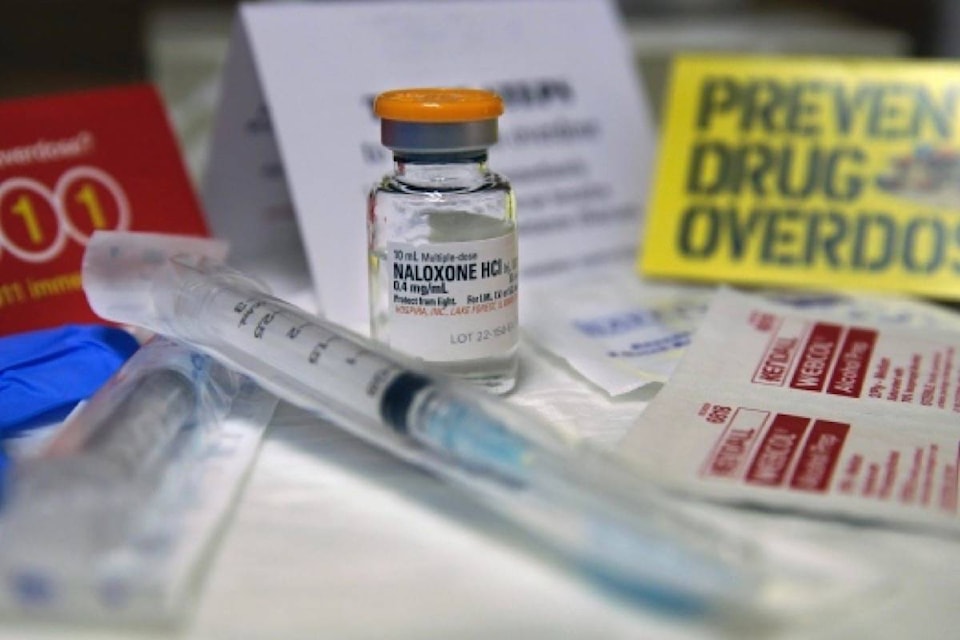
Further, health authorities and not-for-profit groups have hosted workshops on how to administer Naloxone, the overdose-reversing drug, which the government started subsidizing in November. In 2017, Naloxone was administered 14,000 times.
READ MORE: Three new supervised consumption sites approved in B.C.
READ MORE: Pop, candy and now opioids in vending machines?
However, 90 per cent of people who died last year did so while using alone, Lapointe said, illustrating that more needs to be done to reach those who feel too stigmatized to go to safe consumption or overdose prevention sites.
Daly said 2018 will be a year of identifying efforts, community by community.
The top drugs detected in victims, aside from fentanyl, were cocaine, methamphetamines and heroin, according to toxicology tests.
Daly said further solutions will include expanding access to fentanyl test strips, which were distributed late last year and are currently only available at overdose prevention sites.
She said the emergency response centre will begin deploying regional outreach teams, as well.
Kendall makes last call for decriminalization of illicit drugs
On his last day before retirement, Kendall blamed government’s prohibition on drugs as the root cause of fentanyl’s destruction.
A long-term advocate for prescription heroin, Kendall said he watched drug sources change from opium to heroin to fentanyl and now to the even more potent carfentanil, which accounted for 67 deaths in 2017.
READ MORE: B.C. launches emergency response centre to curb overdose deaths
ONE YEAR LATER: B.C.’s first public health emergency continues
Regulations and criminalization have prevented officials from replacing the illegal market with a safer choice, he said.
While he’s seen some changes in the public’s attitude towards the opioid epidemic, Kendall said it’s time to start thinking more broadly, outside of the box and comfort zones, to find methods that save lives.