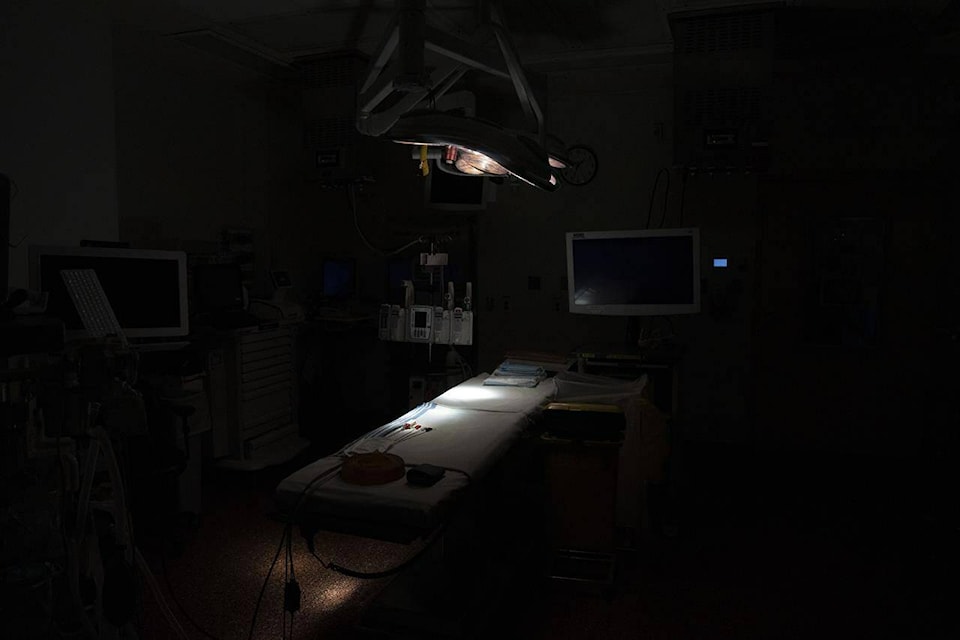
Three large television screens in the nerve centre of the operating room at Canada’s largest pediatric hospital display a list of its surgical spaces, showing which ones have children undergoing procedures at the moment.
There are a lot of blank spots.
Toronto’s Hospital for Sick Children usually runs its operating room at 100 per cent capacity. But on this day, six of its 16 surgical spaces are quiet.
That’s after a massive wave of children with respiratory illnesses flooded the emergency department and overwhelmed the intensive care unit, prompting hospital leadership to make the decision in mid-November to cancel many surgeries.
The hospital needed those specialized staff, especially nurses, to parachute into the emergency department and ICU to help stabilize a precarious situation.
It’s left orthopedic surgeon Dr. Simon Kelley standing in an unusually empty operating room on a recent afternoon.
“It’s eerie,” says the associate chief of perioperative services.
“It’s also heartbreaking because at the same time, an empty operating room is a child who’s not getting their surgery.”
The Canadian Press recently spent hours inside SickKids to better understand the immense challenges faced by pediatric hospitals as they deal with a devastating respiratory illness season. SickKids is among several pediatric hospitals that have had to cancel surgeries, but it is already casting an eye to the future and the catch-up that lies ahead.
The slower pace at the operating room right now is a precursor to a huge wave of surgeries that will need to be conducted when redeployed staff can return once more to their regular roles.
For Kelley, the growing surgical backlog is on his mind all the time.
On the day Kelley spoke to The Canadian Press, there were 6,067 children waiting for various surgeries. That number has since increased to 6,157.
The hospital has cancelled 279 surgeries since the ramp-down order went out in mid-November.
As the wait-list increases, so does staff anxiety.
“There’s a level of distress among health-care workers that we just cannot do what we want to do and what we’re trained to do and provide the surgeries that the children so desperately need,” Kelley says.
The operating room’s clinical manager says the quieter days bring on a different kind of stress.
“Every single time that we slow down, we know we’re affecting the wait-list,” says Laura Matheson.
“We do see how a delay in a lot of these scheduled surgeries impacts the kids.”
The hospital’s worst-case scenario sees this respiratory season lasting until March, which could mean about five months of operating rooms working at 60 per cent capacity.
SickKids conducts emergency surgeries 24 hours a day, with one or two operating rooms on the go overnight. They also typically perform scheduled surgeries from 8 a.m. to 5:30 p.m. on weekdays.
But to catch up on the backlog of surgeries exacerbated by provincial ramp-down orders at the start of the pandemic, the hospital was performing scheduled operations seven days a week on a volunteer basis this year.
They worked at 100 per cent capacity – upwards of 250 surgeries per week.
“Despite that, the wait-list still increased by 15 per cent,” Kelley says. “We can go over and above and do more than we normally do, but that’s going to require a lot more people.”
Right now, Kelley and the hospital have ideas on how to tackle the backlog but plans haven’t been firmed up.
They could work into the evenings and on weekends and would like to be able to conduct even more surgeries if they can secure new operating space. But Kelley says the entire system needs an overhaul.
“We really need to be looking at a system-wide redesign of pediatric care,” Kelley says. “For many years, pediatric care has been underfunded, so this is not a problem that’s just occurred in the last two weeks.”
The hospital would like to implement a true “hub-and-spoke” model with SickKids at the centre and community hospitals with them. That would involve a centralized wait-list system so children can be seen by the first available surgical team.
“That would help us expand our workforce, which would be huge,” he says. “But that’s quite an undertaking.”
The province has said the status quo in the health-care system is not working and they are taking steps to change it.
For now, those working in the operating rooms at SickKids have to keep making difficult choices.
Surgeons have had to figure out whose operation will be cancelled and keep a running priority list.
Emergencies are dealt with first – anything where life or limb is threatened. Then there are urgent surgeries that need to be done within the next two to three weeks, otherwise those children would be harmed.
Those that were cancelled included head, neck and spine surgeries; bone and joint surgeries; and plastic reconstructive surgeries.
“These are all important surgeries, but it’s now a true triage system and unfortunately it means that many of the children on the wait-list will not be getting surgery for some time,” Kelley says.
The results of that triage were sent to administrative co-ordinators who had the unenviable task of informing families.
Karinna Knox made many of those phone calls. She’s the main contact for families before and after surgery, so it’s easy to become close to stressed-out parents.
“It does get really emotional for us, too,” she says. “We feel awful that we’re doing this.”
She starts with the bad news first, then explains the reason for the delay. Then she listens.
The phone calls are intense.
“Emotions range from outright anger to tears to shock,” Knox says.
“I get really close to these families, we talk a lot. So when I’m just ripping that rug out from under them, it’s hard.”
The tough work of telling families of the mass cancellations is largely complete. Now Knox is fielding phone calls about future plans. The unknown for families is just as bad as the cancellation, she says.
The situation has left Knox in a place where she now tells her husband not to talk to her for a bit after her workday ends. She needs silence and time to decompress from delivering bad news to families who could use some good news.
“It’s just really heavy,” she says. “I just do nothing for a bit to make sure that the next day I can be that compassionate, empathetic person that these families need.”
She hopes to deliver some good news soon.
—Liam Casey, The Canadian Press
INSIDE SICK KIDS: An overworked emergency department prepares for a new surge
INSIDE SICK KIDS: How one Canadian pediatric hospital’s ICU was saved from near collapse