Health officials in British Columbia have reported that 45 per cent of those who tested positive for COVID-19 have now recovered from the virus – a stat far greater than any other province in Canada to date.
But that is in part because B.C. has chosen to determine who no longer has the virus differently than other provinces seeing the lion’s share of cases, such as Ontario, Alberta and Quebec.
Provincial health officer Dr. Bonnie Henry said during her daily COVID-19 media briefing on Saturday, March 28, that if a person with the novel coronavirus only exhibits mild symptoms and doesn’t have to be hospitalized then they are determined to be recovered once they’ve reached 10 days without showing any symptoms.
READ MORE: B.C. COVID-19 cases rise 92 to 884, one more death, 81 in care
“That has been validated around the world from data we have seen, particularly from Germany, which shows that after a period of time when your symptoms resolve you no longer shed live virus,” Henry explained.
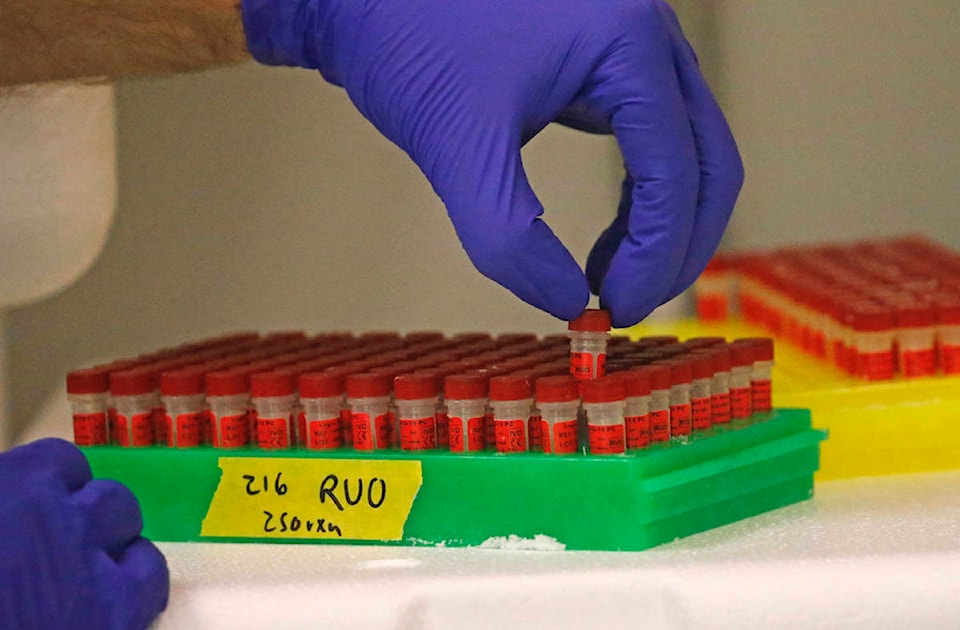
COVID-19 testing is done through a nasopharyngeal swab or throat swab, and looks for the RNA (ribonucleic acid) of the virus, which carries the genetic information of the virus.
But even when someone is no longer infectious, a test will often still detect that RNA, Henry said.
“That RNA may be a symptom of a virus that is no longer alive and you shed it for a period of time in your saliva and sometimes in your stool.”
READ MORE: Mission man with COVID-19 symptoms forced to call 811 more than 100 times
Those who are hospitalized or are immunocompromised are considered recovered once they produce two negative lab tests 24 hours apart – the method that B.C. was using when the first few hundred cases were confirmed.
As of March 28, nearly half – or 396 people – of the 885 confirmed cases in B.C. have recovered. There have been 17 deaths – mainly linked to care home outbreaks, bringing the total number of active cases to 471.
Meanwhile, Ontario has only reported eight cases as resolved, with 1,126 active confirmed cases and 18 fatalities. Thirty-three people have recovered in Alberta, where there are currently 507 active confirmed cases and two deaths.
Ontario is currently relying solely on negative tests to confirm which patients have recovered, but Henry said officials there are considering implementing B.C.’s new testing model.
In Quebec, which has seen the most total confirmed cases of 2,498, only one person has recovered. There, 22 people have died.
The other reason B.C.’s recovery rate is higher is because the province saw more cluster cases sooner, Henry said, pointing to the outbreaks in the Lower Mainland long-term care homes.
“Many of the people affected were young, healthy health-care workers so they had milder disease that didn’t last as long,” she said.
The incubation period for COVID-19 is up to 14 days, according to the B.C. Centre for Disease Control, but because there is no cure, recovery is reliant on a person’s immune system to fight the virus.
READ MORE: Think you have COVID-19? Here is what to do next
B.C.’s testing strategy still focusing on the elderly, high-risk
B.C.’s testing strategy continues to focus on identifying the chains of transmissions while swabbing the elderly, and those with underlying health complications which make them high-risk to seeing adverse symptoms and healthcare workers.
“There is some testing of people if there are clusters being identified in communities – and this is happening all over the province right now,” she said, using the example of an elderly person living with someone who has COVID-19.
B.C. is not yet in the phase where swabbing asymptomatic people is necessary.
“A broad testing of well people in our community right is not what we are going to be doing,” Henry said, but added that this could be a strategy health officials consider as they start to see a decline in the number of cases linked to specific clusters or outbreaks as a way to find new community transmissions and import cases from other provinces.
@ashwadhwani
ashley.wadhwani@bpdigital.ca
Like us on Facebook and follow us on Twitter.